Health
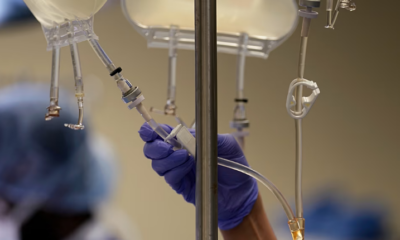
Women’s Health Funding Falls Far Short Despite Major Disease Burden, WEF Report Finds
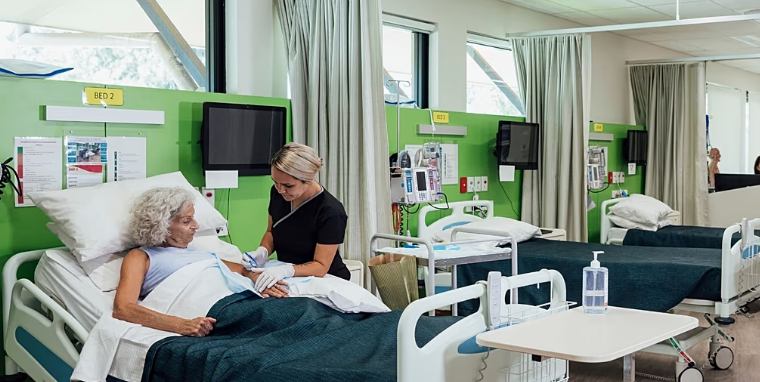
Collectively, women lose approximately 75 million years of healthy life each year – equivalent to a week of health lost per woman annually, according to a new report highlighting persistent gaps in healthcare investment. While women and girls make up 49 percent of the global population and generally live longer than men, they spend 25 percent more of their lives in poor health or living with a disability.
The report, released jointly by the World Economic Forum (WEF) and Boston Consulting Group (BCG), found that investment in women’s health remains disproportionately low and narrowly concentrated on a few areas. Private healthcare funding directed at women’s health accounts for just six percent of total investment, with companies focused exclusively on women attracting less than one percent.
Trish Stroman from BCG and Shyam Bishen from WEF noted in the report that, while gender equality has progressed, “the gap between health outcomes for men and women remains substantial.” In health technology, the disparity is even wider. Analysis by international financial services firm Alantra found that women’s health companies captured only two percent of the $41.2 billion (€35.1 billion) in venture health-tech funding in 2023.
Research suggests that targeted screening and care for four key conditions in the United States – menopause, osteoporosis, Alzheimer’s disease, and cardiovascular disease – could unlock more than $100 billion (€85 billion) in market value. Yet, limited funding, combined with gaps in research design, clinical data, and access to care, continues to entrench this divide. “The result is not only a public-health shortfall but a market inefficiency on a historic scale,” the report stated.
Women face a disproportionate disease burden. Conditions such as endometriosis, menopause, polycystic ovarian syndrome, and certain cancers affect women uniquely. Five gender-specific conditions – endometriosis, maternal health, premenstrual syndrome, menopause, and cervical cancer – represent 14 percent of the female disease burden but have received less than one percent of research funding in recent years.
Between 2020 and 2025, private-sector healthcare funding totaled $2.87 trillion (€2.45 trillion), of which women’s health received just $175 billion (€149 billion). Funding is heavily concentrated in reproductive health, women’s cancers, and maternal care, which together account for 80 percent of identified funding events and 90 percent of capital. By contrast, conditions such as endometriosis, menopause, polycystic ovary syndrome, and menstrual health received less than two percent of the women’s health budget.
The report highlights the need for stronger evidence to drive investment and innovation. Women remain underrepresented in clinical trials, with Harvard Medical School researchers finding that women made up only 41.2 percent of participants in 1,433 trials, despite representing a larger share of the affected populations.
Sania Nishtar of Gavi, the Vaccine Alliance, told a panel at the World Economic Forum in Davos 2026 that innovation must be paired with delivery capability and sustainable financing. “If you do not have that delivery capability and the sustainable financing, you’re unable to use innovations for the impact that they’re intended to have,” she said.
The report calls for targeted, cross-sector leadership and a deeper understanding of women’s health to translate scientific evidence into meaningful policy and care solutions.
Health
Genetic Differences May Shape Effectiveness of Popular Weight-Loss Drugs, Study Finds
Health
Seven-Day Meditation Retreat Linked to Measurable Changes in Brain and Body, Study Finds
Health
Uzbekistan to Launch Nationwide State Medical Insurance System in 2026
Uzbekistan will begin introducing a nationwide state medical insurance system from 2026, part of a broader overhaul of the country’s healthcare financing and service delivery. The reform will introduce digital referrals, a national health insurance fund, and a guaranteed package of essential medical services funded through the state budget. Officials say the changes aim to improve efficiency, expand access, and reduce informal payments.
“State health insurance is a social protection system designed to guarantee access to quality healthcare services,” said Zokhid Ermatov, executive director of the State Health Insurance Fund.
Discussions about state medical insurance in Uzbekistan began in 2017, but implementing such a system required years of preparation. The State Health Insurance Fund was formally established in December 2020, and pilot programmes launched in the Syrdarya region in 2021 tested new financing mechanisms, regulatory frameworks, and digital health systems. In November 2025, the Cabinet of Ministers approved regulations governing how medical care funded through the state budget will be provided in public and private medical institutions, with the rules set to come into force on January 1, 2026.
At the centre of the new model is stronger primary healthcare. Patients will first visit their assigned family clinic, where doctors provide consultations, prescribe tests, and determine whether specialist care is needed. If necessary, patients will receive an electronic referral to hospitals or specialists. Emergency and urgent care will remain available without referrals.
The reform introduces a patient-centred financing model, where healthcare providers are paid by the State Health Insurance Fund based on services delivered. Primary healthcare will be funded through capitation payments, while hospital treatment will follow case-based payments, a structure designed to improve efficiency and treatment outcomes.
A fully digital referral system will allow patients to choose hospitals from a list of institutions contracted with the State Health Insurance Fund using a government portal or mobile app. Referrals will remain valid for 60 days, and waiting lists and hospitalisations will be managed through a unified electronic health information system.
The insurance system guarantees essential healthcare services, including family doctor consultations, diagnostic tests, outpatient treatment, preventive screening, some medicines, hospital care, and certain rehabilitation services. Patients will not be charged additional fees for services included in the approved package.
Funding for the program will come primarily from the state budget, ensuring citizens do not pay direct insurance contributions. Priority access will be given to socially vulnerable groups, including children with disabilities, orphans, pensioners, pregnant women, unemployed citizens, and low-income families. The State Health Insurance Fund will allocate resources across regions to strengthen medical services and reduce inequalities.
International organisations have praised Uzbekistan’s approach, noting that general tax financing and universal coverage can improve financial protection and ensure predictable healthcare funding. Jessika Yin, Health Policy Adviser at the World Health Organization in Uzbekistan, said the reforms align with global trends toward universal health coverage.
If implemented successfully, Uzbekistan’s state medical insurance system could represent a major step toward universal healthcare, ensuring that people receive care without facing financial hardship.
-

 Entertainment2 years ago
Entertainment2 years agoMeta Acquires Tilda Swinton VR Doc ‘Impulse: Playing With Reality’
-

 Business2 years ago
Business2 years agoSaudi Arabia’s Model for Sustainable Aviation Practices
-

 Business2 years ago
Business2 years agoRecent Developments in Small Business Taxes
-

 Home Improvement1 year ago
Home Improvement1 year agoEffective Drain Cleaning: A Key to a Healthy Plumbing System
-

 Politics2 years ago
Politics2 years agoWho was Ebrahim Raisi and his status in Iranian Politics?
-

 Sports2 years ago
Sports2 years agoChina’s Historic Olympic Victory Sparks National Pride Amid Controversy
-

 Business2 years ago
Business2 years agoCarrectly: Revolutionizing Car Care in Chicago
-

 Sports2 years ago
Sports2 years agoKeely Hodgkinson Wins Britain’s First Athletics Gold at Paris Olympics in 800m