Health
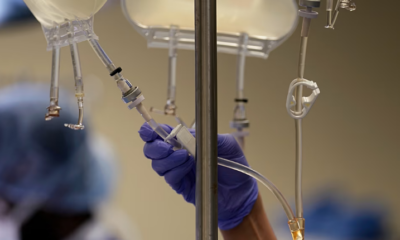
Sugar Drops Can Reduce Pain for Babies During Needle Procedures, Study Finds
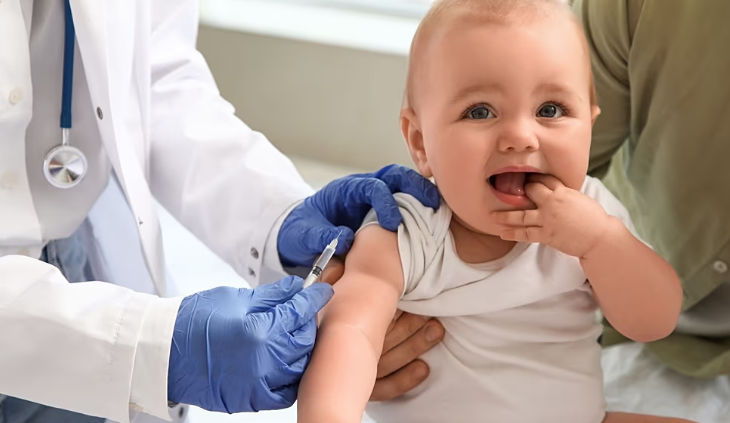
A simple dose of sugar placed in a baby’s mouth before a needle procedure can significantly reduce pain, according to a new scientific review. The findings, published by researchers from the University of Toronto and the University of Ottawa, suggest that sucrose may offer an effective, low-cost way to comfort newborns and infants undergoing routine medical procedures.
Infants, particularly those in neonatal and pediatric intensive care units, frequently undergo procedures such as vaccinations, blood tests, or intravenous line insertions. Because their pain regulation systems are still developing, babies can experience pain more intensely than adults, making effective pain relief crucial.
The review, conducted by the Cochrane Collaboration, analyzed 29 trials involving 2,764 babies worldwide. In each study, infants were randomly assigned to receive either sugar solution, other pain relief methods such as pacifiers, breastfeeding, skin-to-skin contact, or no intervention. Researchers found that sugar reduced pain both during and immediately after needle procedures. In comparison, sugar appeared to provide more immediate relief than pacifiers alone.
“Parents may be surprised to learn that something as simple as a few drops of sugar solution can make a real difference to their baby’s comfort during blood tests,” said Ligyana Candido, co-author of the study from the University of Ottawa.
The study highlighted that while sugar is effective in the short term, its benefits compared with breastfeeding or skin-to-skin care remain less clear, due to limited evidence. Still, sugar offers a practical alternative, especially in situations where other comforting methods are unavailable.
Hospitalized newborns, including premature babies or those receiving treatment for specific conditions, are often exposed to repeated needle procedures. The review noted that untreated pain during these early stages of life can negatively affect growth and development. “Newborn babies undergo frequent needle procedures in hospital without any pain relief or comforting measures, even though older children and adults rarely have these procedures done without pain care,” said lead author Mariana Bueno from the University of Toronto.
Researchers emphasized that sugar works quickly, usually within minutes, and can be easily administered at a low cost. However, they cautioned that the long-term effects of repeated sucrose use in infants require further study.
“The message from our findings is ultimately that infants need and should receive pain management before a procedure such as venepuncture,” Bueno added.
The review provides strong evidence supporting the use of sugar as a safe and effective method to ease procedural pain in babies, potentially improving the hospital experience for both infants and their parents.
Health
Genetic Differences May Shape Effectiveness of Popular Weight-Loss Drugs, Study Finds
Health
Seven-Day Meditation Retreat Linked to Measurable Changes in Brain and Body, Study Finds
Health
Uzbekistan to Launch Nationwide State Medical Insurance System in 2026
Uzbekistan will begin introducing a nationwide state medical insurance system from 2026, part of a broader overhaul of the country’s healthcare financing and service delivery. The reform will introduce digital referrals, a national health insurance fund, and a guaranteed package of essential medical services funded through the state budget. Officials say the changes aim to improve efficiency, expand access, and reduce informal payments.
“State health insurance is a social protection system designed to guarantee access to quality healthcare services,” said Zokhid Ermatov, executive director of the State Health Insurance Fund.
Discussions about state medical insurance in Uzbekistan began in 2017, but implementing such a system required years of preparation. The State Health Insurance Fund was formally established in December 2020, and pilot programmes launched in the Syrdarya region in 2021 tested new financing mechanisms, regulatory frameworks, and digital health systems. In November 2025, the Cabinet of Ministers approved regulations governing how medical care funded through the state budget will be provided in public and private medical institutions, with the rules set to come into force on January 1, 2026.
At the centre of the new model is stronger primary healthcare. Patients will first visit their assigned family clinic, where doctors provide consultations, prescribe tests, and determine whether specialist care is needed. If necessary, patients will receive an electronic referral to hospitals or specialists. Emergency and urgent care will remain available without referrals.
The reform introduces a patient-centred financing model, where healthcare providers are paid by the State Health Insurance Fund based on services delivered. Primary healthcare will be funded through capitation payments, while hospital treatment will follow case-based payments, a structure designed to improve efficiency and treatment outcomes.
A fully digital referral system will allow patients to choose hospitals from a list of institutions contracted with the State Health Insurance Fund using a government portal or mobile app. Referrals will remain valid for 60 days, and waiting lists and hospitalisations will be managed through a unified electronic health information system.
The insurance system guarantees essential healthcare services, including family doctor consultations, diagnostic tests, outpatient treatment, preventive screening, some medicines, hospital care, and certain rehabilitation services. Patients will not be charged additional fees for services included in the approved package.
Funding for the program will come primarily from the state budget, ensuring citizens do not pay direct insurance contributions. Priority access will be given to socially vulnerable groups, including children with disabilities, orphans, pensioners, pregnant women, unemployed citizens, and low-income families. The State Health Insurance Fund will allocate resources across regions to strengthen medical services and reduce inequalities.
International organisations have praised Uzbekistan’s approach, noting that general tax financing and universal coverage can improve financial protection and ensure predictable healthcare funding. Jessika Yin, Health Policy Adviser at the World Health Organization in Uzbekistan, said the reforms align with global trends toward universal health coverage.
If implemented successfully, Uzbekistan’s state medical insurance system could represent a major step toward universal healthcare, ensuring that people receive care without facing financial hardship.
-

 Entertainment2 years ago
Entertainment2 years agoMeta Acquires Tilda Swinton VR Doc ‘Impulse: Playing With Reality’
-

 Business2 years ago
Business2 years agoSaudi Arabia’s Model for Sustainable Aviation Practices
-

 Business2 years ago
Business2 years agoRecent Developments in Small Business Taxes
-

 Home Improvement1 year ago
Home Improvement1 year agoEffective Drain Cleaning: A Key to a Healthy Plumbing System
-

 Politics2 years ago
Politics2 years agoWho was Ebrahim Raisi and his status in Iranian Politics?
-

 Sports2 years ago
Sports2 years agoChina’s Historic Olympic Victory Sparks National Pride Amid Controversy
-

 Business2 years ago
Business2 years agoCarrectly: Revolutionizing Car Care in Chicago
-

 Sports2 years ago
Sports2 years agoKeely Hodgkinson Wins Britain’s First Athletics Gold at Paris Olympics in 800m