Health
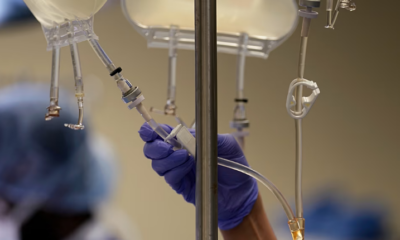
Europe Faces Growing Challenges in Meeting Medical Care Needs, EU Report Shows

A new report has highlighted stark disparities in healthcare access across Europe, revealing that a growing number of citizens face unmet medical needs due to systemic issues such as high costs and long waiting times.
According to the latest data from Eurostat and the Health at a Glance: Europe 2024 report, 3.8 per cent of EU residents aged 16 and over reported unmet medical needs in the past year. However, the percentage climbs significantly when focusing solely on individuals who actively required healthcare services — with some countries reporting unmet needs among over 20 per cent of this group.
The causes are twofold: healthcare system barriers, including long waiting lists and treatment costs, account for 2.4 per cent of all cases, while 1.4 per cent stem from personal reasons such as fear of doctors, lack of time, or lack of knowledge about available care.
Unmet healthcare needs vary widely across the continent. Estonia tops the list within the EU, with 15.5 per cent of people reporting unmet needs, followed closely by Greece and Albania, each over 13 per cent. Even wealthier Nordic countries show surprising figures — Denmark (12.2 per cent), Finland, and Norway (over 7.5 per cent) — despite high healthcare spending. Conversely, countries such as Germany (0.5 per cent), Austria (1.3 per cent), and the Netherlands (1.4 per cent) report the lowest levels, pointing to more efficient and accessible healthcare systems.
Cost is a dominant barrier in nations like Greece and Albania, where over 9 per cent of citizens cited unaffordable care. In contrast, long waiting times are the primary issue in countries like Estonia (12 per cent) and Finland (7.5 per cent).
Income inequality also plays a major role. On average, 3.8 per cent of low-income individuals across the EU report unmet needs due to healthcare system issues — more than triple the 1.2 per cent reported by higher-income groups. In Greece, that gap is particularly wide, with 23 per cent of low-income respondents affected.
Healthcare experts say these disparities reflect more than just economic factors. Dr. Tit Albreht, President of the European Public Health Association (EUPHA), noted, “Unmet health needs arise from different reasons, including how well healthcare governance integrates services to meet population needs.”
Industry leaders, such as Tina Taube of the European Federation of Pharmaceutical Industries and Associations (EFPIA), stressed the importance of timely access to diagnosis and treatment. “Unmet needs are context-specific,” she said. “It’s not just about product availability, but also healthcare system readiness.”
Andy Powrie-Smith of EFPIA added that patients in some European countries wait up to seven times longer than others for the same treatments due to regulatory delays and varying national infrastructures.
The findings underscore the need for a more coordinated, equitable healthcare strategy across the continent, especially as Europe faces the challenges of an ageing population and increasingly complex medical technologies.
Health
Genetic Differences May Shape Effectiveness of Popular Weight-Loss Drugs, Study Finds
Health
Seven-Day Meditation Retreat Linked to Measurable Changes in Brain and Body, Study Finds
Health
Uzbekistan to Launch Nationwide State Medical Insurance System in 2026
Uzbekistan will begin introducing a nationwide state medical insurance system from 2026, part of a broader overhaul of the country’s healthcare financing and service delivery. The reform will introduce digital referrals, a national health insurance fund, and a guaranteed package of essential medical services funded through the state budget. Officials say the changes aim to improve efficiency, expand access, and reduce informal payments.
“State health insurance is a social protection system designed to guarantee access to quality healthcare services,” said Zokhid Ermatov, executive director of the State Health Insurance Fund.
Discussions about state medical insurance in Uzbekistan began in 2017, but implementing such a system required years of preparation. The State Health Insurance Fund was formally established in December 2020, and pilot programmes launched in the Syrdarya region in 2021 tested new financing mechanisms, regulatory frameworks, and digital health systems. In November 2025, the Cabinet of Ministers approved regulations governing how medical care funded through the state budget will be provided in public and private medical institutions, with the rules set to come into force on January 1, 2026.
At the centre of the new model is stronger primary healthcare. Patients will first visit their assigned family clinic, where doctors provide consultations, prescribe tests, and determine whether specialist care is needed. If necessary, patients will receive an electronic referral to hospitals or specialists. Emergency and urgent care will remain available without referrals.
The reform introduces a patient-centred financing model, where healthcare providers are paid by the State Health Insurance Fund based on services delivered. Primary healthcare will be funded through capitation payments, while hospital treatment will follow case-based payments, a structure designed to improve efficiency and treatment outcomes.
A fully digital referral system will allow patients to choose hospitals from a list of institutions contracted with the State Health Insurance Fund using a government portal or mobile app. Referrals will remain valid for 60 days, and waiting lists and hospitalisations will be managed through a unified electronic health information system.
The insurance system guarantees essential healthcare services, including family doctor consultations, diagnostic tests, outpatient treatment, preventive screening, some medicines, hospital care, and certain rehabilitation services. Patients will not be charged additional fees for services included in the approved package.
Funding for the program will come primarily from the state budget, ensuring citizens do not pay direct insurance contributions. Priority access will be given to socially vulnerable groups, including children with disabilities, orphans, pensioners, pregnant women, unemployed citizens, and low-income families. The State Health Insurance Fund will allocate resources across regions to strengthen medical services and reduce inequalities.
International organisations have praised Uzbekistan’s approach, noting that general tax financing and universal coverage can improve financial protection and ensure predictable healthcare funding. Jessika Yin, Health Policy Adviser at the World Health Organization in Uzbekistan, said the reforms align with global trends toward universal health coverage.
If implemented successfully, Uzbekistan’s state medical insurance system could represent a major step toward universal healthcare, ensuring that people receive care without facing financial hardship.
-

 Entertainment2 years ago
Entertainment2 years agoMeta Acquires Tilda Swinton VR Doc ‘Impulse: Playing With Reality’
-

 Business2 years ago
Business2 years agoSaudi Arabia’s Model for Sustainable Aviation Practices
-

 Business2 years ago
Business2 years agoRecent Developments in Small Business Taxes
-

 Home Improvement1 year ago
Home Improvement1 year agoEffective Drain Cleaning: A Key to a Healthy Plumbing System
-

 Politics2 years ago
Politics2 years agoWho was Ebrahim Raisi and his status in Iranian Politics?
-

 Sports2 years ago
Sports2 years agoChina’s Historic Olympic Victory Sparks National Pride Amid Controversy
-

 Business2 years ago
Business2 years agoCarrectly: Revolutionizing Car Care in Chicago
-

 Sports2 years ago
Sports2 years agoKeely Hodgkinson Wins Britain’s First Athletics Gold at Paris Olympics in 800m