Health
UK Researchers Prepare NHS Trial for Nitrous Oxide as Rapid Depression Treatment
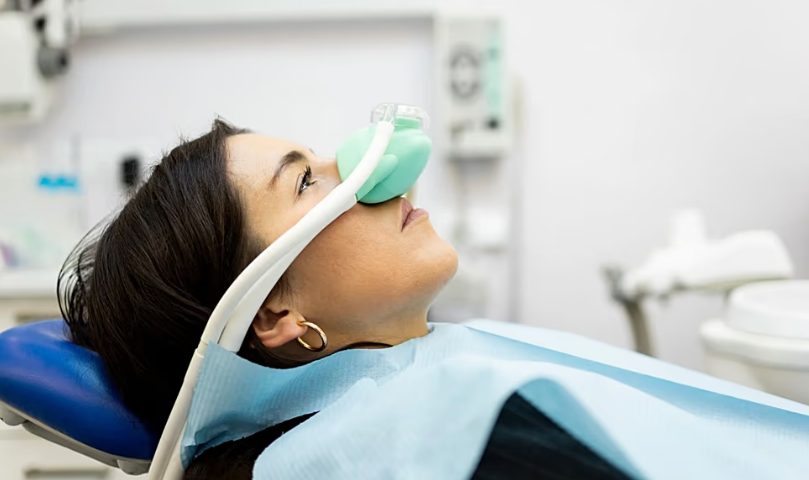
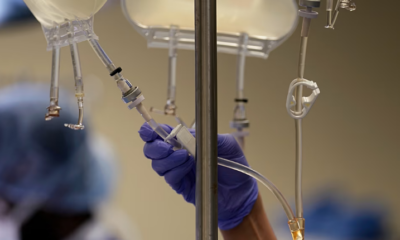
Researchers at the University of Birmingham are preparing the first National Health Service (NHS) trial to test whether nitrous oxide, commonly known as “laughing gas,” can be safely and effectively used to treat severe or treatment-resistant depression. The move follows a major analysis combining the strongest clinical evidence to date on the gas’s potential antidepressant effects.
The study, published in eBioMedicine, examined how medically administered nitrous oxide (N₂O) affects adults with major depressive disorder (MDD) and treatment-resistant depression (TRD). TRD is typically diagnosed when patients fail to respond to at least two standard antidepressants, a situation affecting almost half of UK patients, earlier research indicates.
The analysis found that a single session inhaling 50 percent nitrous oxide produced significant reductions in depressive symptoms within 24 hours. These effects, however, were often short-lived, generally fading within a week. Repeated sessions appeared to provide more lasting improvements, echoing findings from studies on ketamine, another fast-acting treatment thought to influence similar glutamate pathways in the brain.
“Depression is a debilitating illness, made even more challenging by the fact that standard antidepressants do not provide meaningful relief for nearly half of patients,” said Kiranpreet Gill, PhD researcher at the University of Birmingham and lead author of the report. “This study consolidates the best available evidence suggesting that nitrous oxide can offer rapid and clinically significant short-term relief for patients with severe depression.”
While side effects such as nausea, dizziness, and headaches were relatively common, they were generally brief and no immediate safety concerns were identified. Researchers caution that the long-term effects of repeated nitrous oxide use remain largely unknown, and the limited number of trials makes it difficult to draw firm conclusions at this stage.
The work is part of the NIHR-funded Mental Health Mission Midlands Translational Centre, which aims to improve care for patients with severe and treatment-resistant depression. The upcoming NHS trial will assess whether nitrous oxide can be delivered safely and acceptably in clinical settings, potentially adding a new option to the growing field of rapid-acting depression treatments.
Gill added that larger trials will be necessary to determine safe, repeatable dosing strategies and to evaluate the long-term outcomes for patients. If successful, nitrous oxide could become an important addition to current therapeutic options, offering fast relief for those who do not benefit from conventional antidepressants.
Health
Genetic Differences May Shape Effectiveness of Popular Weight-Loss Drugs, Study Finds
Health
Seven-Day Meditation Retreat Linked to Measurable Changes in Brain and Body, Study Finds
Health
Uzbekistan to Launch Nationwide State Medical Insurance System in 2026
Uzbekistan will begin introducing a nationwide state medical insurance system from 2026, part of a broader overhaul of the country’s healthcare financing and service delivery. The reform will introduce digital referrals, a national health insurance fund, and a guaranteed package of essential medical services funded through the state budget. Officials say the changes aim to improve efficiency, expand access, and reduce informal payments.
“State health insurance is a social protection system designed to guarantee access to quality healthcare services,” said Zokhid Ermatov, executive director of the State Health Insurance Fund.
Discussions about state medical insurance in Uzbekistan began in 2017, but implementing such a system required years of preparation. The State Health Insurance Fund was formally established in December 2020, and pilot programmes launched in the Syrdarya region in 2021 tested new financing mechanisms, regulatory frameworks, and digital health systems. In November 2025, the Cabinet of Ministers approved regulations governing how medical care funded through the state budget will be provided in public and private medical institutions, with the rules set to come into force on January 1, 2026.
At the centre of the new model is stronger primary healthcare. Patients will first visit their assigned family clinic, where doctors provide consultations, prescribe tests, and determine whether specialist care is needed. If necessary, patients will receive an electronic referral to hospitals or specialists. Emergency and urgent care will remain available without referrals.
The reform introduces a patient-centred financing model, where healthcare providers are paid by the State Health Insurance Fund based on services delivered. Primary healthcare will be funded through capitation payments, while hospital treatment will follow case-based payments, a structure designed to improve efficiency and treatment outcomes.
A fully digital referral system will allow patients to choose hospitals from a list of institutions contracted with the State Health Insurance Fund using a government portal or mobile app. Referrals will remain valid for 60 days, and waiting lists and hospitalisations will be managed through a unified electronic health information system.
The insurance system guarantees essential healthcare services, including family doctor consultations, diagnostic tests, outpatient treatment, preventive screening, some medicines, hospital care, and certain rehabilitation services. Patients will not be charged additional fees for services included in the approved package.
Funding for the program will come primarily from the state budget, ensuring citizens do not pay direct insurance contributions. Priority access will be given to socially vulnerable groups, including children with disabilities, orphans, pensioners, pregnant women, unemployed citizens, and low-income families. The State Health Insurance Fund will allocate resources across regions to strengthen medical services and reduce inequalities.
International organisations have praised Uzbekistan’s approach, noting that general tax financing and universal coverage can improve financial protection and ensure predictable healthcare funding. Jessika Yin, Health Policy Adviser at the World Health Organization in Uzbekistan, said the reforms align with global trends toward universal health coverage.
If implemented successfully, Uzbekistan’s state medical insurance system could represent a major step toward universal healthcare, ensuring that people receive care without facing financial hardship.
-

 Entertainment2 years ago
Entertainment2 years agoMeta Acquires Tilda Swinton VR Doc ‘Impulse: Playing With Reality’
-

 Business2 years ago
Business2 years agoSaudi Arabia’s Model for Sustainable Aviation Practices
-

 Business2 years ago
Business2 years agoRecent Developments in Small Business Taxes
-

 Home Improvement1 year ago
Home Improvement1 year agoEffective Drain Cleaning: A Key to a Healthy Plumbing System
-

 Politics2 years ago
Politics2 years agoWho was Ebrahim Raisi and his status in Iranian Politics?
-

 Sports2 years ago
Sports2 years agoChina’s Historic Olympic Victory Sparks National Pride Amid Controversy
-

 Business2 years ago
Business2 years agoCarrectly: Revolutionizing Car Care in Chicago
-

 Sports2 years ago
Sports2 years agoKeely Hodgkinson Wins Britain’s First Athletics Gold at Paris Olympics in 800m