Health
Managing Dry Eyes After Cataract Surgery
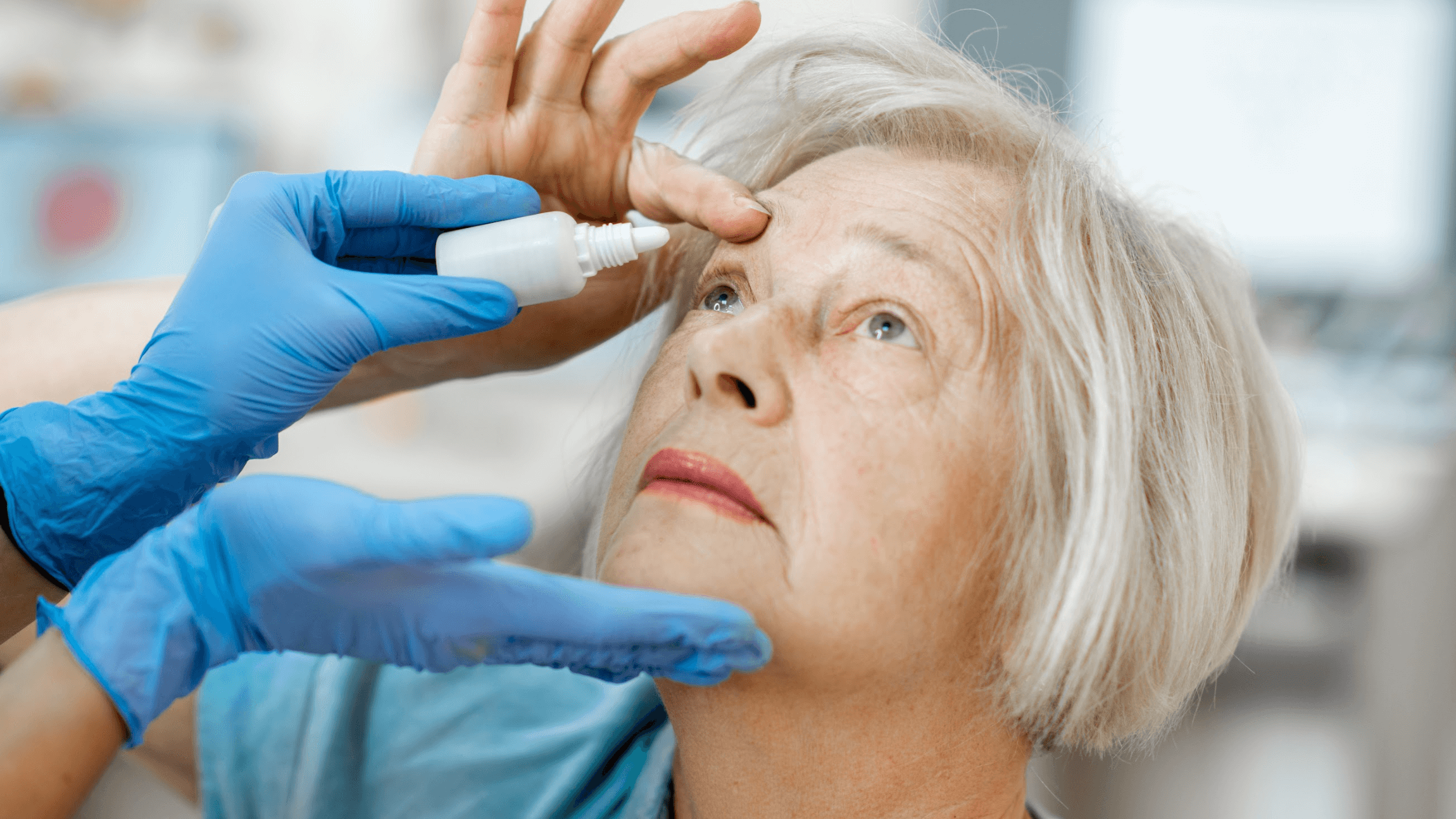
Cataract surgery is one of the most common and successful procedures performed to restore vision clarity. However, like any surgical procedure, it can have side effects, with dry eyes being one of the most frequent. This condition occurs when the surgery disrupts the tear film balance on the eye’s surface. The cornea, crucial for maintaining eye moisture, can have its nerve endings affected during the procedure. These nerve endings are responsible for signaling the body to produce tears, and when disrupted, the eye may not receive the necessary lubrication, leading to dryness and discomfort.
While this side effect is typically temporary, it can cause significant discomfort, including a gritty or burning sensation, and may even impact vision sharpness during recovery. Understanding this potential outcome and knowing how to manage it is essential for a smoother recovery and optimal results from cataract surgery.
Causes
Dry eyes after cataract surgery can be attributed to several factors. One of the primary causes is nerve damage. During cataract surgery, small incisions are made in the cornea, which can temporarily affect the nerves responsible for signaling tear production. This disruption can lead to reduced tear production, leaving the eye feeling dry and uncomfortable.
Another contributing factor is the medication prescribed post-surgery. Antibiotic eye drops, commonly used to prevent infection, can sometimes exacerbate dryness by altering the tear film or reducing the eye’s natural moisture. For those who already suffer from dry eye syndrome, these medications can further intensify the symptoms, making the recovery period more challenging.
Pre-existing dry eye is also a significant consideration. Individuals with dry eye before surgery are at a higher risk of experiencing more severe dryness afterward. The combination of pre-existing conditions and surgical side effects can lead to increased discomfort, emphasizing the importance of managing dry eye symptoms before and after cataract surgery.
Symptoms
After cataract surgery, many patients may notice symptoms indicating the presence of dry eyes, which can be both uncomfortable and disruptive. For instance, Ronald, a 67-year-old patient, began experiencing a persistent feeling of dryness and grit in his eye, almost as if a foreign particle was irritating the surface. This sensation was accompanied by a burning feeling, making it difficult for him to keep his eyes open for extended periods.
Ronald also noticed blurred vision, particularly in the afternoons, which interfered with his ability to read. The unstable tear film on his eye’s surface made it challenging to focus on tasks requiring sharp vision. Additionally, Ronald dealt with significant eye fatigue, feeling as though his eyes were overworked even after short periods of activity. His sensitivity to light, known as photophobia, further complicated his daily life, prompting him to wear sunglasses indoors. Recognizing these symptoms, Ronald consulted his doctor, who provided strategies to manage his dry eyes, ultimately improving his comfort during recovery.
Treatment and Management
Most cases of dry eyes after cataract surgery improve within a few months as the corneal nerves heal. During this period, managing the symptoms is crucial. Artificial tears over-the-counter lubricating eye drops can provide immediate relief from dryness and irritation. For those needing something stronger, prescription eye drops may be recommended by a doctor to help restore moisture and reduce inflammation.
Warm compresses can also be beneficial. Applying a warm compress to the eyes stimulates tear production and soothes irritation. Additionally, eye exercises, such as regular blinking or focusing on distant objects, can help improve tear distribution and reduce eye strain.
Minimizing exposure to environmental irritants like smoke, wind, and dry environments is essential to prevent further aggravation of symptoms. Creating a comfortable environment for your eyes as they heal is important.
If dry eye symptoms persist or worsen, it’s crucial to consult an eye doctor. They can evaluate the condition and recommend appropriate treatment options to ensure smooth recovery.
While dry eyes after cataract surgery can be uncomfortable, understanding the causes and symptoms, along with effective treatment and management strategies, can significantly improve recovery. By using artificial tears, applying warm compresses, performing eye exercises, and avoiding irritants, you can alleviate symptoms and support the eyes’ natural healing process. Addressing dry eyes promptly will help ensure the full benefits of cataract surgery, leading to clearer vision and a more comfortable daily life.
Health
Global Mental Health Cases Near 1.2 Billion as Anxiety and Depression Drive Sharp Worldwide Rise

A major global analysis has found that mental health conditions have surged to an estimated 1.2 billion people worldwide, driven largely by steep increases in anxiety and depression over the past three decades.
The findings, published in The Lancet as part of the Global Burden of Disease Study 2023, show that the number of people living with mental disorders has almost doubled since 1990, marking a 95% rise. Researchers say major depressive disorder and anxiety disorders have seen even sharper growth, increasing by 131% and 158% respectively, making them the most prevalent mental health conditions globally.
The report describes mental illnesses as widespread conditions that create long-term disability and significant human suffering. It also highlights broader consequences for economies and public services, including reduced productivity, lower workforce participation and increasing pressure on health and welfare systems.
Researchers estimate that in 2023 alone, around 620 million females and 552 million males were affected by mental health conditions. While the overall burden is rising across both sexes, the study points to notable differences in the types and prevalence of disorders.
Among women, depression and anxiety were the most commonly reported conditions, alongside higher rates of eating disorders such as anorexia nervosa and bulimia nervosa. The report links this disparity to a mix of biological, social and structural factors, including exposure to domestic violence, sexual abuse, gender inequality and reproductive health-related changes.
In contrast, neurodevelopmental and behavioural disorders, including attention deficit hyperactivity disorder (ADHD), conduct disorder and autism spectrum conditions, were more frequently diagnosed in men.
Teenagers aged 15 to 19 were identified as the group experiencing the highest mental health burden globally, raising concerns about early onset of conditions and insufficient preventive care for young people.
The study identifies several key risk factors associated with mental illness, including childhood sexual violence, bullying and intimate partner violence. These factors are strongly linked to conditions such as depression, schizophrenia, bipolar disorder and anxiety disorders. However, researchers note that such exposures have remained relatively stable over time and account for only a portion of the overall rise.
According to the authors, broader drivers are likely contributing to the increasing prevalence of mental disorders. These include genetic and biological influences, poverty, inequality, and the growing impact of global crises such as armed conflict, pandemics, natural disasters and climate-related stress.
While mental health conditions have long been a leading cause of disability worldwide, the report warns that the situation is worsening. At the same time, health systems have not expanded services at a pace matching demand.
The authors caution that the gap between rising need and limited access to care is becoming more pronounced, leaving millions without adequate treatment or support.
Health
Europe Records Sharp Rise in Sexually Transmitted Infections, ECDC Warns
Health
White House Rejects Report It Blocked Return of Ebola-Infected US Doctor
-

 Entertainment2 years ago
Entertainment2 years agoMeta Acquires Tilda Swinton VR Doc ‘Impulse: Playing With Reality’
-

 Sports2 years ago
Sports2 years agoChina’s Historic Olympic Victory Sparks National Pride Amid Controversy
-

 Business2 years ago
Business2 years agoSaudi Arabia’s Model for Sustainable Aviation Practices
-

 Business2 years ago
Business2 years agoRecent Developments in Small Business Taxes
-

 Home Improvement1 year ago
Home Improvement1 year agoEffective Drain Cleaning: A Key to a Healthy Plumbing System
-

 Politics2 years ago
Politics2 years agoWho was Ebrahim Raisi and his status in Iranian Politics?
-

 Sports2 years ago
Sports2 years agoKeely Hodgkinson Wins Britain’s First Athletics Gold at Paris Olympics in 800m
-

 Business2 years ago
Business2 years agoCarrectly: Revolutionizing Car Care in Chicago