Health
Drug Repurposing in Cancer Treatment: Emerging Strategies and Promising Developments

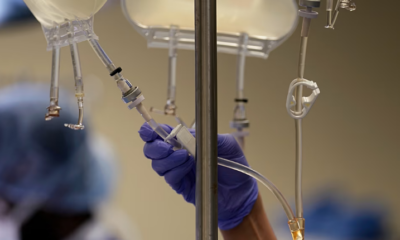
Cancer continues to be one of the leading causes of death globally, with millions of new diagnoses each year. The conventional process of developing new cancer drugs is notoriously slow and costly, often requiring more than a decade and billions of dollars to reach patients. In response, drug repurposing, also called drug repositioning, has gained significant attention as a practical alternative. This strategy finds new anticancer applications for medications already approved for other medical conditions. Because these drugs have established safety records, known dosing guidelines, and existing production methods, repurposing can dramatically shorten development timelines and lower financial barriers compared with creating entirely new compounds. Organizations focused on innovative and integrative oncology approaches, such as Sanare Lab, offer valuable insights and resources for exploring experimental protocols in this rapidly evolving field.
One especially interesting avenue within drug repurposing is methylene blue cancer research. This compound, long used as a dye and as a treatment for methemoglobinemia, is now under investigation for possible anticancer effects. Researchers have examined methylene blue in photodynamic therapy, where it serves as a photosensitizer. When activated by specific wavelengths of light, it generates reactive oxygen species that can damage and kill cancer cells. Laboratory and animal studies have shown reductions in tumor volume in models of colorectal cancer, breast cancer, and melanoma, particularly when combined with other treatment approaches. These findings illustrate how a familiar, inexpensive compound might provide new ways to target resistant or difficult-to-treat tumors.
Why Drug Repurposing Matters in Oncology
The main advantage of repurposing lies in its efficiency. Traditional drug discovery begins with identifying a new molecule, followed by years of laboratory testing, animal studies, and multi-phase human trials to confirm both safety and effectiveness. Repurposed drugs skip much of this early work because regulators have already approved them for their original use. Investigators can therefore move more quickly to testing whether the drug works against cancer, often starting directly in mid- or late-stage clinical trials.
Cost is another critical factor. The failure rate in new oncology drug development frequently exceeds ninety percent, driving up expenses that are eventually reflected in treatment prices. Many repurposed candidates are off-patent generics, which means they can be produced and distributed at a fraction of the cost of branded medicines. With cancer rates expected to keep rising worldwide, especially in low- and middle-income countries, affordable options derived from existing drugs could help close gaps in access to effective care.
Well-Known Examples of Repurposed Drugs in Cancer
Drug repurposing already has several important successes in oncology. Thalidomide, originally marketed as a sedative and later withdrawn because of severe birth defects, was rediscovered in the late 1990s for multiple myeloma. Its ability to block new blood vessel formation in tumors made it a valuable addition to treatment regimens, and it remains widely used today, frequently combined with other agents.
All-trans retinoic acid, first studied for skin conditions, transformed outcomes in acute promyelocytic leukemia by prompting malignant cells to mature into normal ones. When paired with arsenic trioxide, another agent with a long history in traditional medicine, the combination now achieves very high remission rates in this once-deadly subtype of leukemia.
Metformin, the most commonly prescribed medication for type 2 diabetes, has attracted attention after population studies showed lower cancer rates among diabetic patients taking it. The drug appears to interfere with energy metabolism in cancer cells by activating a key regulatory pathway that slows uncontrolled growth. Multiple clinical trials have tested metformin as an add-on to standard chemotherapy or radiation in breast, prostate, colorectal, and other cancers, with some studies reporting improved survival or reduced recurrence.
Statins, best known for lowering cholesterol, have also been evaluated for anticancer effects. By blocking an enzyme involved in cholesterol synthesis, they disrupt signaling pathways that cancer cells use to grow and spread. Large observational studies have linked statin use to modestly reduced risk of certain cancers, and ongoing research continues to explore their role as adjunctive therapy.
Other candidates include antiparasitic agents such as mebendazole, which interfere with the structural framework cancer cells need to divide, and the anticonvulsant valproic acid, which modifies gene expression by inhibiting enzymes that control DNA packaging. Both have shown activity in laboratory models of colorectal, brain, and pancreatic cancers, and early human studies are underway.
Spotlight on Methylene Blue in Cancer Research
Returning to methylene blue, this compound continues to generate interest because of its diverse biological effects. Beyond its role in photodynamic therapy, methylene blue can influence cancer cell metabolism. Many tumors depend heavily on glycolysis for energy production even when oxygen is available, a phenomenon known as the Warburg effect. Methylene blue appears to disrupt this altered metabolism, potentially starving cancer cells of fuel. In preclinical models of ovarian cancer, particularly those resistant to platinum-based chemotherapy, methylene blue slowed tumor progression more effectively than standard drugs in some experiments.
When used in photodynamic therapy, methylene blue tends to concentrate in mitochondria, the energy-producing structures inside cells. Light exposure then triggers the release of damaging oxygen radicals, leading to cell death through apoptosis. Systematic reviews of animal studies have reported consistent tumor shrinkage across several cancer types, including breast carcinoma and skin melanoma, often with low toxicity at the doses tested.
Methylene blue may also improve tumor oxygenation, which could make radiotherapy more effective. Poorly oxygenated regions within solid tumors are notoriously resistant to radiation, so any agent that increases oxygen availability has therapeutic potential. In addition, surgeons sometimes use methylene blue injections to map sentinel lymph nodes during breast cancer operations, helping to identify the first nodes where cancer is most likely to spread.
Despite these encouraging signals, methylene blue remains experimental for most cancer applications. While side effects are generally mild at therapeutic doses, interactions with certain medications require careful monitoring. Large, well-controlled clinical trials are still needed to determine whether the promising laboratory and early human data translate into meaningful benefits for patients.
Remaining Challenges and the Path Forward
Drug repurposing is not without obstacles. Because many candidate drugs are generic, pharmaceutical companies have limited financial incentive to fund expensive trials for new indications. Regulatory agencies sometimes require nearly as much evidence for a repurposed use as for a completely novel drug, which can slow progress. Off-label prescribing also raises questions about informed consent and standardized protocols when robust data are lacking.
Collaborative efforts are helping to address these barriers. Networks of researchers, clinicians, and advocacy groups are systematically reviewing existing drugs for anticancer potential, prioritizing those with the strongest preclinical rationale, and pushing for well-designed trials. Advances in computational biology allow scientists to screen thousands of compounds against cancer-related targets much faster than before, narrowing the list of drugs worth testing in the laboratory or clinic.
Looking ahead, combination strategies are likely to dominate. Pairing repurposed agents with immunotherapy, targeted therapies, or conventional chemotherapy could produce synergistic effects greater than any single treatment alone. Personalized approaches that match specific drugs to the molecular features of an individual’s tumor will further refine their use.
In summary, drug repurposing offers a realistic and increasingly important strategy for improving cancer care. From established successes like thalidomide and metformin to emerging candidates such as methylene blue, the field demonstrates that familiar medicines can sometimes deliver unexpected benefits against one of medicine’s toughest challenges. Sustained investment in rigorous clinical research and broader collaboration will determine how much further this approach can take us toward more effective, accessible treatments for patients everywhere.
Health
Genetic Differences May Shape Effectiveness of Popular Weight-Loss Drugs, Study Finds
Health
Seven-Day Meditation Retreat Linked to Measurable Changes in Brain and Body, Study Finds
Health
Uzbekistan to Launch Nationwide State Medical Insurance System in 2026
Uzbekistan will begin introducing a nationwide state medical insurance system from 2026, part of a broader overhaul of the country’s healthcare financing and service delivery. The reform will introduce digital referrals, a national health insurance fund, and a guaranteed package of essential medical services funded through the state budget. Officials say the changes aim to improve efficiency, expand access, and reduce informal payments.
“State health insurance is a social protection system designed to guarantee access to quality healthcare services,” said Zokhid Ermatov, executive director of the State Health Insurance Fund.
Discussions about state medical insurance in Uzbekistan began in 2017, but implementing such a system required years of preparation. The State Health Insurance Fund was formally established in December 2020, and pilot programmes launched in the Syrdarya region in 2021 tested new financing mechanisms, regulatory frameworks, and digital health systems. In November 2025, the Cabinet of Ministers approved regulations governing how medical care funded through the state budget will be provided in public and private medical institutions, with the rules set to come into force on January 1, 2026.
At the centre of the new model is stronger primary healthcare. Patients will first visit their assigned family clinic, where doctors provide consultations, prescribe tests, and determine whether specialist care is needed. If necessary, patients will receive an electronic referral to hospitals or specialists. Emergency and urgent care will remain available without referrals.
The reform introduces a patient-centred financing model, where healthcare providers are paid by the State Health Insurance Fund based on services delivered. Primary healthcare will be funded through capitation payments, while hospital treatment will follow case-based payments, a structure designed to improve efficiency and treatment outcomes.
A fully digital referral system will allow patients to choose hospitals from a list of institutions contracted with the State Health Insurance Fund using a government portal or mobile app. Referrals will remain valid for 60 days, and waiting lists and hospitalisations will be managed through a unified electronic health information system.
The insurance system guarantees essential healthcare services, including family doctor consultations, diagnostic tests, outpatient treatment, preventive screening, some medicines, hospital care, and certain rehabilitation services. Patients will not be charged additional fees for services included in the approved package.
Funding for the program will come primarily from the state budget, ensuring citizens do not pay direct insurance contributions. Priority access will be given to socially vulnerable groups, including children with disabilities, orphans, pensioners, pregnant women, unemployed citizens, and low-income families. The State Health Insurance Fund will allocate resources across regions to strengthen medical services and reduce inequalities.
International organisations have praised Uzbekistan’s approach, noting that general tax financing and universal coverage can improve financial protection and ensure predictable healthcare funding. Jessika Yin, Health Policy Adviser at the World Health Organization in Uzbekistan, said the reforms align with global trends toward universal health coverage.
If implemented successfully, Uzbekistan’s state medical insurance system could represent a major step toward universal healthcare, ensuring that people receive care without facing financial hardship.
-

 Entertainment2 years ago
Entertainment2 years agoMeta Acquires Tilda Swinton VR Doc ‘Impulse: Playing With Reality’
-

 Business2 years ago
Business2 years agoSaudi Arabia’s Model for Sustainable Aviation Practices
-

 Business2 years ago
Business2 years agoRecent Developments in Small Business Taxes
-

 Home Improvement1 year ago
Home Improvement1 year agoEffective Drain Cleaning: A Key to a Healthy Plumbing System
-

 Politics2 years ago
Politics2 years agoWho was Ebrahim Raisi and his status in Iranian Politics?
-

 Sports2 years ago
Sports2 years agoChina’s Historic Olympic Victory Sparks National Pride Amid Controversy
-

 Business2 years ago
Business2 years agoCarrectly: Revolutionizing Car Care in Chicago
-

 Sports2 years ago
Sports2 years agoKeely Hodgkinson Wins Britain’s First Athletics Gold at Paris Olympics in 800m