Health
UK Confirms Case of New Mpox Strain Amid Rising European Concerns
The United Kingdom has reported a new case of the highly contagious mpox clade Ib strain, becoming the latest European country to document an infection amid rising global concern over the virus’s spread.
The UK Health Security Agency confirmed that the newly identified patient had not travelled recently and had no known link to previously confirmed cases, suggesting possible local transmission. Authorities have traced the individual’s close contacts, but no additional cases have been reported. Health officials say the overall public risk remains low.
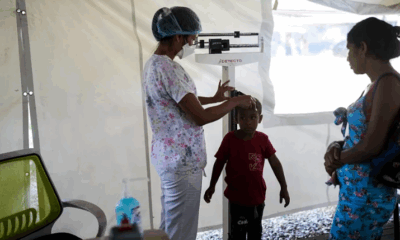
The new strain, known as clade Ib, first emerged in the Democratic Republic of the Congo (DRC) in 2023 and has since caused thousands of infections across Central Africa, particularly in Burundi and Uganda. While two major subtypes of mpox exist, Clade I, predominant in Central Africa, is considered more severe than Clade II, which triggered a global outbreak in 2022 and remains active at low levels in parts of Europe and North America.
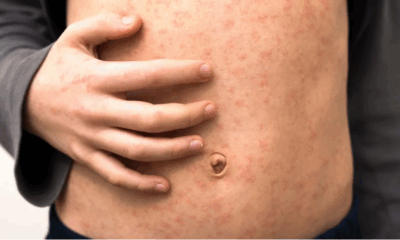
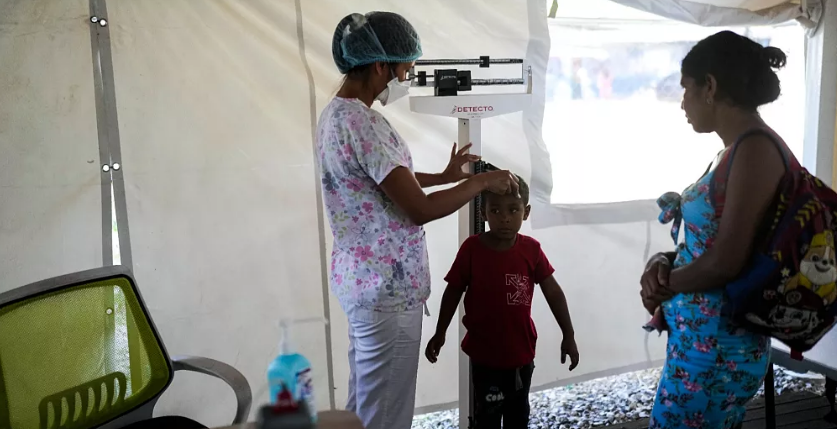
Clade Ib has proven particularly troubling for public health experts due to its potential for easier transmission and more severe illness, particularly among children. Mpox spreads through close skin-to-skin contact and can cause symptoms such as fever, rash, swollen lymph nodes, headaches, and respiratory issues. In August 2024, the World Health Organization declared the African mpox outbreak a global public health emergency.
Following early warnings, the UK prepared for potential transmission by securing more than 150,000 doses of mpox vaccines and establishing vaccination sites across England. The country’s first clade Ib cases were reported in October 2024, involving a returning traveller who subsequently infected household members.
Elsewhere in Europe, several countries have reported cases of the clade Ib strain. Germany has confirmed eight cases to date, including household transmissions among children, while Belgium has recorded five cases since December. France reported two cases earlier this year linked to individuals returning from Central Africa.
Sweden was the first non-African country to detect the new strain, reporting a case in August 2024 involving a patient who had recently travelled to an affected area. Ireland has documented one case of the related but distinct clade Ia strain in February, involving a traveller from the DRC who was hospitalised in Dublin.
Globally, the new strain has also been identified in the United States, Canada, Brazil, China, India, Thailand, Oman, Pakistan, Qatar, and the United Arab Emirates, highlighting the virus’s increasing international footprint.
European health officials continue to monitor developments closely. While the risk to the general public remains low, experts stress the importance of preparedness, including vaccination and early detection, as the virus continues to spread beyond Africa.
Health
Early-Onset Cancer Rates Rising in U.S., But Deaths Mostly Stable, Study Finds

A new U.S. government study has revealed that while cancer diagnoses among people under 50 are on the rise, the overall death rates for most types of cancer in this age group remain stable.
Published Thursday in the journal Cancer Discovery, the study is one of the most comprehensive assessments to date of early-onset cancers, analyzing data from more than two million cases diagnosed in Americans aged 15 to 49 between 2010 and 2019.
The findings show that 14 out of 33 cancer types had increasing incidence rates in at least one younger age group. The most significant increases were seen in breast, colorectal, kidney, and uterine cancers. Women accounted for about 63 percent of the early-onset cases.
“This pattern generally reflects something profound going on,” said Tim Rebbeck of the Dana-Farber Cancer Institute, who was not involved in the study. “We need to fund research that will help us understand why this is happening.”
The study found that, compared to 2010 data, there were 4,800 more breast cancer cases, 2,000 additional colorectal cancers, 1,800 more kidney cancers, and 1,200 extra uterine cancers by 2019.
Despite the rising numbers, researchers emphasized a key reassurance: death rates for most of these cancers are not increasing. However, exceptions were noted—colorectal, uterine, and testicular cancers saw slight rises in mortality among younger adults.
The causes behind the rise in early-onset cancers are not fully understood. The study’s datasets do not include information on potential risk factors such as obesity, lifestyle, or access to healthcare. However, researchers, including lead author Dr. Meredith Shiels of the National Cancer Institute, highlighted obesity as a possible driver.
“Several of these cancer types are known to be associated with excess body weight,” said Dr. Shiels. She also pointed to advances in detection and changing screening practices as possible contributors to earlier diagnoses.
Breast cancer trends may also be influenced by shifting reproductive patterns, such as women having children later in life, which has been associated with increased cancer risk due to fewer years of pregnancy and breastfeeding—factors known to lower risk.
Not all cancer types followed the upward trend. Rates of more than a dozen cancers, including lung and prostate cancer, are decreasing among younger people. Researchers attribute the lung cancer decline to reduced smoking rates, while updated PSA screening guidelines are likely behind the drop in prostate cancer diagnoses.
Experts plan to convene later this year to further investigate the growing early-onset cancer burden and explore targeted prevention strategies.
Health
UK Scientists Develop Tool to Measure ‘Heart Age,’ Offering New Insights for Cardiovascular Health

Researchers in the United Kingdom have developed a new tool that can determine how old a person’s heart is in comparison to their actual age, offering a potential breakthrough in the early detection and prevention of cardiovascular disease.
The study, led by scientists at the University of East Anglia (UEA), examined magnetic resonance imaging (MRI) scans from 557 individuals across the UK, Spain, and Singapore. Of those, 336 participants had known health risk factors such as obesity, high blood pressure, or diabetes.
Using these scans, the researchers measured structural and functional markers of cardiac health — including the size of the heart’s chambers and how effectively it pumps blood. These indicators were then used to create an algorithm that calculates the heart’s “functional age.”
The findings, published in the European Heart Journal, revealed that individuals with cardiovascular risk factors had hearts that were, on average, 4.6 years older than their chronological age. In people with obesity, the gap was even wider, indicating faster cardiac ageing.
“People with health issues like diabetes or obesity often have hearts that are ageing faster than they should – sometimes by decades,” said Dr. Pankaj Garg, a cardiologist and lead author of the study. “This tool gives us a way to visualize and quantify that risk.”
While the tool shows promise, researchers noted some limitations. The model does not account for how long patients had lived with their conditions, and the study group primarily included older individuals who had survived with these health issues — raising concerns about survivor bias. The relatively small sample size also means the tool needs broader validation before it can be widely adopted.
Despite these limitations, the research team believes the tool could have valuable clinical applications in the future. Dr. Garg said it may help doctors counsel patients more effectively about their cardiovascular health and recommend lifestyle changes or treatments to slow heart ageing.
“By knowing your heart’s true age, patients could get advice or treatments to slow down the ageing process, potentially preventing heart attacks or strokes,” he said. “It’s about giving people a fighting chance against heart disease.”
The team hopes the tool could eventually be integrated into routine care, empowering patients to take early steps toward improving their heart health through diet, exercise, and medical intervention.
Health
Global Health Inequities Persist as Progress on Life Expectancy and Mortality Slows, Says WHO
-

 Business12 months ago
Business12 months agoSaudi Arabia’s Model for Sustainable Aviation Practices
-

 Business12 months ago
Business12 months agoRecent Developments in Small Business Taxes
-

 Politics12 months ago
Politics12 months agoWho was Ebrahim Raisi and his status in Iranian Politics?
-

 Business10 months ago
Business10 months agoCarrectly: Revolutionizing Car Care in Chicago
-

 Business10 months ago
Business10 months agoSaudi Arabia: Foreign Direct Investment Rises by 5.6% in Q1
-

 Technology12 months ago
Technology12 months agoComparing Apple Vision Pro and Meta Quest 3
-

 Politics12 months ago
Politics12 months agoIndonesia and Malaysia Call for Israel’s Compliance with ICJ Ruling on Gaza Offensive
-

 Technology12 months ago
Technology12 months agoRecent Developments in AI Ethics in America